October 6, 2015 - Multiparametric MRI (mpMRI) and targeted prostate biopsy improve the accuracy of systematic biopsy to select patients for active surveillance, according to a recent study.1
Active surveillance is the preferred management strategy for men with low-risk prostate cancer. Challenges in this field include improving patient selection, optimizing follow-up strategies, and identifying appropriate triggers for intervention. Advances in mpMRI have lead to improved detection of prostate tumors, and MRI has emerged as a tool to monitor men on active surveillance.
The researchers reviewed the latest developments in mpMRI to monitor active surveillance patients and describe areas of future research.
In recent findings, mpMRI targeted prostate biopsy results in a higher detection rate of significant prostate cancer, and a lower probability of detecting insignificant tumors, compared to systematic biopsy.
The research also found mpMRI-targeted biopsies have improved diagnosis of significant anterior tumors. A small proportion of high-grade tumors is missed by mpMRI and targeted biopsy. However, the majority of these tumors are small-volume, Gleason grade 3 + 4 cancers, and their clinical significance is unknown.
The authors concluded pMRI and targeted prostate biopsy have emerged as tools to improve the accuracy of systematic biopsy to select patients for active surveillance. The role of mpMRI to monitor and trigger intervention in these patients is understudied, and integration of MRI data with clinical characteristics can help many men avoid routine confirmatory biopsy.
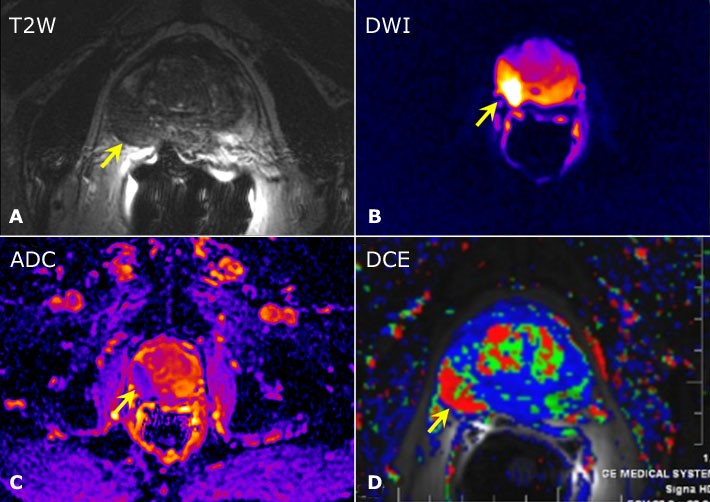
Image: Axial Multiparametric MR Images. A) T2-weighted, B) diffusion weighted (DWI), C) apparent diffusion coefficient (ADC) and D) dynamic contrast enhanced (DCE) images of a patient with prostate cancer. The tumor appears dark on the axial T2-weighted image (arrow); the corresponding area shows restricted diffusion on the DWI and ADC images as well as abnormal contrast enhancement on the DCE axial image (as evident from abnormal red color coding of the tumor).2
References:
- Pedro R, Behfar E. The role of MRI in active surveillance for men with localized prostate cancer. Current Opinion in Urology. November 2015 - Volume 25 - Issue 6 - p 504–509. doi: 10.1097/MOU.0000000000000221.
- Miller JC. Multiparametric MR Imaging for Prostate Cancer. Radrounds. Vol. 8, issue 8.




